Appendicitis facts for kids
Quick facts for kids Appendicitis |
|
|---|---|
| Synonyms | Epityphlitis |
| Symptoms | Periumbilical or right lower abdominal pain, vomiting, nausea, decreased appetite, high fever |
| Complications | Abdominal inflammation, sepsis, Gastrointestinal bleeding, gastrointestinal abscess |
| Diagnostic method | Based on symptoms, medical imaging, blood tests |
| Similar conditions | Mesenteric adenitis, cholecystitis, psoas abscess, abdominal aortic aneurysm |
| Treatment | Surgical removal of the appendix, antibiotics |
| Frequency | 11.6 million (2015) |
| Deaths | 50,100 (2015) |
Appendicitis is when your appendix gets swollen and infected. The appendix is a small, finger-shaped pouch that sticks out from your large intestine. Common signs include pain in the lower right side of your belly, feeling sick to your stomach, throwing up, a fever, and not wanting to eat. Sometimes, people don't have these usual signs. If the appendix bursts, it can cause serious problems like a bad infection in your belly.
Contents
Why Does Appendicitis Happen?
Appendicitis usually starts when the opening of your appendix gets blocked. This blockage can happen for several reasons:
- Hardened stool: Doctors call this an appendicolith or fecalith.
- Swollen lymph tissue: Sometimes, the tissue inside the appendix swells up. This can happen after a viral infection.
- Other blockages: Less often, things like tiny parasites or even small growths can block the appendix.
When the appendix is blocked, it fills with mucus and swells. This causes pressure inside. The pressure also reduces blood flow to the appendix. Then, bacteria that live naturally in the gut start to grow quickly. This leads to infection and inflammation.
If the blockage and infection are not treated, the appendix tissue can get damaged and start to die. Bacteria can then leak out of the appendix walls. This can cause a pocket of infection (pus) around the appendix. If the appendix bursts, it releases bacteria into the belly. This can lead to a very serious infection called peritonitis, which can be dangerous.
Some research suggests that eating a diet low in fiber might play a role. Fiber helps keep your digestive system moving smoothly.
How Do Doctors Find Out if You Have Appendicitis?
Doctors usually figure out if you have appendicitis by asking about your symptoms and doing a physical check-up. If they're not sure, they might use special tests. These tests include medical imaging (like scans) and blood tests.
What Are the Signs and Symptoms?
The main signs of appendicitis are sudden belly pain, feeling sick, throwing up, and a fever.
- Belly Pain: The pain often starts as a dull ache around your belly button. After a few hours, it usually moves to the lower right side of your belly. This area then becomes very sore. The pain can get worse when you move, cough, or press on your belly.
- Other Symptoms: You might also feel nauseous, throw up, or lose your appetite. A mild fever is also common.
Doctors look for specific signs during an exam:
- McBurney's Point:
This is a spot on your lower right belly that becomes very tender when pressed.
- Dunphy's Sign: If you feel more pain in your lower right belly when you cough, it's called Dunphy's sign.
- Psoas Sign: Pain when you straighten your right leg or lift your right knee.
- Rovsing's Sign: Pain in your lower right belly when a doctor presses on the lower left side.
Sometimes, the appendix is in a different position, which can change where you feel the pain.
Lab Tests
Doctors often order blood tests to check for signs of infection.
- White Blood Cell Count (WBC): A high WBC count can mean your body is fighting an infection.
- C-reactive protein (CRP): This blood test helps find out if there's inflammation in your body.
- Urinalysis: This urine test helps rule out a urinary tract infection that could cause similar belly pain.
- Pregnancy Test: For girls, a pregnancy test is important to rule out other causes of abdominal pain.
Imaging Scans
Imaging tests help doctors see inside your body.
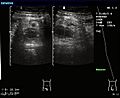
- Ultrasound: This uses sound waves to create pictures of your appendix. It's often the first choice for kids and pregnant women because it doesn't use radiation. Ultrasound can show if the appendix is swollen or if there's fluid around it.
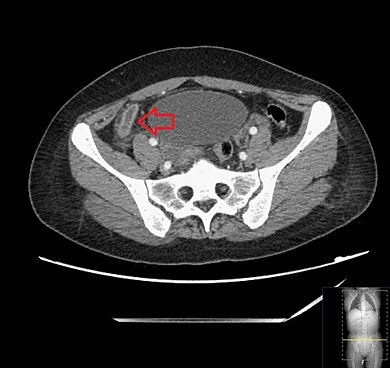
- CT Scan: A CT scan uses X-rays to create detailed pictures. It's very accurate for diagnosing appendicitis in adults and older teens.
- MRI: MRI uses strong magnets and radio waves. It's also used for kids and pregnant patients when an ultrasound isn't clear, as it avoids radiation.
Scoring Systems
Doctors sometimes use a scoring system, like the Alvarado score, to help decide if someone has appendicitis. It gives points for different symptoms and test results. A higher score means appendicitis is more likely.
| Migratory right iliac fossa pain | 1 point |
| Anorexia (loss of appetite) | 1 point |
| Nausea and vomiting | 1 point |
| Right iliac fossa tenderness | 2 points |
| Rebound abdominal tenderness | 1 point |
| Fever | 1 point |
| High white blood cell count (leukocytosis) | 2 points |
| Shift to left (segmented neutrophils) | 1 point |
| Total score | 10 points |
|---|
Other Conditions That Cause Similar Pain
Many other conditions can cause belly pain that feels like appendicitis. Doctors consider these possibilities:
- In children: Stomach flu, swollen lymph nodes in the belly, or other bowel problems.
- In girls: Problems with the ovaries or other pelvic organs can cause similar pain.
- In adults: Gallbladder problems, kidney stones, or other digestive issues.
How is Appendicitis Treated?
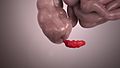
The main treatment for appendicitis is surgery to remove the appendix. This surgery is called an appendectomy. Surgeons can do this in two ways:
- Open surgery: This uses one larger cut in your belly.
- Laparoscopic surgery: This uses a few small cuts and a tiny camera.
Surgery is very important to prevent the appendix from bursting. Sometimes, if the appendicitis is not severe, doctors might try antibiotics first. However, many people treated with antibiotics still need surgery later. Appendicitis is a common reason for sudden belly pain that needs surgery. In 2015, about 11.6 million people had appendicitis, and about 50,100 people died from it worldwide.
Before Surgery
Before surgery, you won't be allowed to eat or drink for a while. You'll get fluids through an IV drip in your arm. Antibiotics are often given to help prevent infection. You'll also receive medicine for pain and nausea. The surgeon will explain the procedure and any risks.
Types of Surgery
- Open Appendectomy:
This is the traditional way to remove the appendix. The surgeon makes one cut, usually about 2 to 3 inches long, in the lower right side of your belly. They remove the appendix and then close the cut with stitches or staples.
- Laparoscopic Appendectomy:
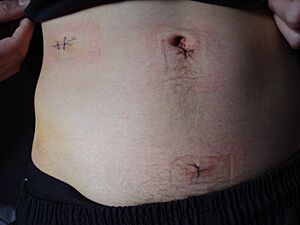
This is a less invasive method. The surgeon makes three or four small cuts, each about 0.25 to 0.5 inches long. A special tool called a laparoscope, which has a tiny camera, is inserted through one cut. This lets the surgeon see inside your belly on a monitor. Other small tools are used through the other cuts to remove the appendix. This method often leads to less pain and a faster recovery.
- Laparoscopic-assisted transumbilical appendectomy: This is a newer technique, especially for kids. The appendix is removed through a single cut near the belly button. This can result in good healing and a small scar.
After Surgery
After surgery, you'll be watched closely as you wake up from general anesthesia. You'll get pain medicine if you need it. Doctors will encourage you to sit up and walk a little bit each day. This helps with recovery. You'll usually start with clear liquids and then move to a regular diet as your body heals.
The time you spend in the hospital can vary. If your appendix didn't burst, you might go home in a day or two. If it did burst, you might stay longer. Full recovery usually takes about 4 to 6 weeks. It's important to follow your doctor's advice and limit physical activity during this time.
What Happens After Treatment?
Most people recover quickly after their appendix is removed. However, complications can happen if treatment is delayed. Recovery time depends on your age and how severe the appendicitis was. It usually takes a few weeks to feel completely better.
If appendicitis is not treated quickly, it can lead to serious infections like peritonitis. This is why it's important to see a doctor right away if you think you have appendicitis.
Sometimes, if the appendix infection isn't too bad, it might get better on its own. But doctors often recommend removing it anyway to prevent it from coming back.
A Look Back in Time: History of Appendicitis
Doctors have known about the appendix for a long time, but they didn't always understand appendicitis. The appendix was first described in the 1500s. Over the centuries, doctors learned more about it.
The term "appendicitis" was first used by an American doctor named Reginald Heber Fitz in 1886. This helped doctors around the world understand and talk about the condition better. Soon after, Dr. Charles McBurney identified McBurney's point, the tender spot on the belly. Modern surgery techniques for removing the appendix developed in the early 1900s.
A famous case happened in 1902 when Edward VII, the King of England, had appendicitis just before his coronation. His successful surgery helped people understand that appendicitis could be treated.
Who Gets Appendicitis?
Appendicitis is most common in people between the ages of 5 and 40. In 2013, about 72,000 people worldwide died from appendicitis.
In the United States, appendicitis is one of the most common reasons for kids aged 5-17 to visit the emergency room and need to stay in the hospital.
Images for kids
-
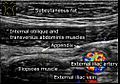
Location of the appendix in the digestive system.
-
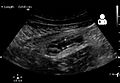
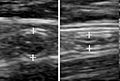
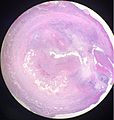
An ultrasound image of acute appendicitis in December 2008.
-
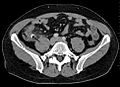
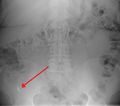
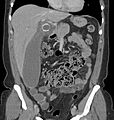
Coronal CT scan of an enlarged inflamed gallbladder that reaches the right lower part of the abdomen.
See also
 In Spanish: Apendicitis para niños
In Spanish: Apendicitis para niños
- Evan O'Neill Kane
- Leonid Rogozov