Cataract surgery facts for kids
Quick facts for kids Cataract surgery |
|
|---|---|
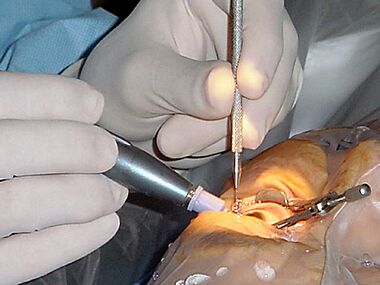
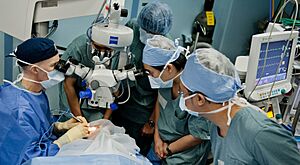
Cataract surgery, using a temporal approach phacoemulsification probe (in right hand) and "chopper" (in left hand)
|
|
| Specialty | Ophthalmology |
| ICD-9-CM | 13.19 |
| MeSH | D002387 |
| MedlinePlus | 002957 |
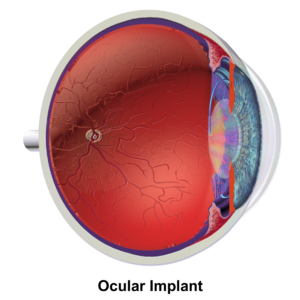
Cataract surgery, also known as lens replacement surgery, is a common operation. It involves removing the natural lens of your eye when it has become cloudy. This cloudy area is called a cataract. After removing the cloudy lens, doctors usually replace it with a clear, artificial intraocular lens (IOL).
Over time, the natural lens in your eye can change and become cloudy. This cloudiness, a cataract, can make it hard to see clearly. Some babies are even born with cataracts. Early signs of a cataract might be bright lights causing a lot of glare or difficulty seeing well in dim light.
During cataract surgery, the cloudy lens is carefully taken out. This is usually done by breaking it up or cutting it out. Then, a new artificial lens (IOL) is put in its place. This new lens helps your eye focus again. An eye doctor (ophthalmologist) usually performs this surgery. It's often done in a clinic or hospital, and you can usually go home the same day. Doctors use local anesthesia, so you won't feel much pain. The surgery is quick, and most people recover enough for daily activities in a few days. Full recovery takes about a month.
More than 90% of these operations successfully help people see better. Serious problems are rare. In many parts of the world, modern surgery uses tiny cuts and quick recovery times. This is the main way cataract surgery is done today.
Contents
Cataract Surgery: Helping You See Clearly
Cataract surgery is the most common way to remove a cloudy lens. It helps when a cataract makes your vision blurry or dim. Cataracts usually grow slowly and can affect one or both eyes. Early signs might include colors looking faded, blurry or double vision, halos around lights, or trouble seeing at night (night blindness). If left untreated, cataracts can lead to blindness. Sometimes, lens removal is part of surgery after an eye injury. The lens is almost always replaced with an artificial one. This is because the natural lens helps your eye focus at different distances.
Cataracts often happen as people get older. But they can also be caused by injuries, radiation exposure, or be present from birth. They can also develop after other eye surgeries. Cataracts form when proteins in the lens clump together. This stops light from reaching the retina at the back of your eye. An eye examination can show if you have cataracts.
Wearing the right glasses can help with early cataract symptoms. But if glasses don't help enough, surgery is the only real treatment. Surgery with new lenses usually leads to better vision and a better quality of life. However, this surgery is not always easy to get in every country.
How is Cataract Surgery Done?
Today, there are two main ways to do cataract surgery: phacoemulsification and extracapsular cataract extraction. Older methods are rarely used now.
In phacoemulsification (often called "phaco"), a special tool uses ultrasonic sound waves. These waves break the cloudy lens into tiny pieces. Then, the pieces are gently sucked out of the eye. A newer version uses a laser to help with some steps. This laser makes the cuts and starts breaking up the lens. Phaco surgery uses a very small cut, so it often doesn't need stitches.
In extracapsular cataract extraction (ECCE) and its variation, manual small incision cataract surgery (MSICS), the lens is removed by hand. It's taken out either whole or in a few large pieces. ECCE uses a larger cut and usually needs stitches. MSICS uses a special cut that often seals itself, so stitches are not needed.
Studies show that MSICS works just as well as phaco for very dense cataracts. MSICS is also faster and costs less. Because of this, MSICS is popular in developing countries. It gives good results, causes less astigmatism, and helps people recover quickly. It's also easier for surgeons to learn and works for almost all types of cataracts.
After the cloudy lens is removed, an artificial lens (IOL) is put in. Small, foldable lenses are used for phaco surgery's tiny cuts. Larger, non-foldable lenses are used for the bigger cuts in extracapsular surgery.
Intracapsular cataract extraction (ICCE) removes the entire lens and its surrounding capsule in one piece. This method has more risks because it needs a large cut. It's rarely done today where modern equipment is available. After ICCE, an IOL can be placed in a different part of the eye.
The oldest known cataract surgery was called couching. This involved pushing the cloudy lens out of the way, but it stayed inside the eye. The eye could not focus well after this. Couching is no longer used in modern medicine.
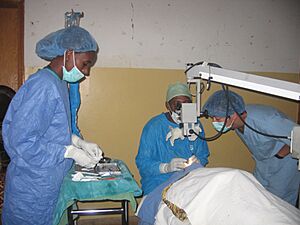
Phacoemulsification is the most common surgery in developed countries. But because phaco machines are expensive, ECCE and MSICS are more common in developing countries. Most cataract surgeries are done as "day-care" procedures. This means you don't stay overnight in the hospital, which saves money.
Preparing for Surgery
Before surgery, your eye doctor will do an eye examination. This confirms you have a cataract and checks if surgery is right for you. They will see how much the cataract affects your vision. If you have other eye problems like age-related macular degeneration or glaucoma, you might still have surgery. But your vision might not improve as much.
Sometimes, a combined surgery for both cataracts and glaucoma can be planned. Your pupil will be widened with eyedrops to help the doctor see the cataract better. If you take certain medicines, like tamsulosin, tell your doctor. These can cause a problem called intraoperative floppy iris syndrome (IFIS) during surgery.
Studies have shown that routine medical tests before surgery don't usually reduce problems during or after the operation. This is compared to surgeries with no or limited pre-op tests.
Some reasons why cataract surgery might not be done include:
- The cataract doesn't affect your vision much.
- You have other serious health problems.
- Surgery won't make your vision better.
- You have advanced macular degeneration or a Detached retina.
- You have an eye infection that needs to be treated first.
- You don't want the surgery.
- Glasses or other aids already help you see well enough.
Choosing Your New Lens (IOL)
After the cataract is removed, an artificial lens (IOL) is usually put in. Foldable IOLs can be put in through a very small cut. Rigid lenses need a larger cut. Foldable IOLs are made of special plastic materials. They are inserted with a special tool. The IOL is usually placed inside the "capsular bag" where the cataract used to be. Sometimes, it might be placed just in front of the capsular bag.
Doctors choose the right IOL power for you. This is like choosing a prescription for glasses. They take measurements of your eye, like its length and the curve of your cornea.
- Monofocal IOLs give clear vision at one distance only (far, middle, or near). You might still need glasses for reading or computer work.
- Multifocal IOLs can focus light from both far and near objects. They work a bit like bifocal glasses. Your doctor will discuss if these are right for you.
- If you need surgery on both eyes, your doctor might suggest monovision. This means one eye gets an IOL for near vision, and the other gets one for distance vision. Most people adjust to this, but some might find both distances blurry.
- Some IOLs are designed to change focus using your eye's natural movements.
- Toric lenses are used to correct astigmatism, which is when your eye has an uneven curve.
- Aspheric IOLs can improve how you see contrast.
- Some IOLs can block ultraviolet and blue light, like your natural lens does.
- Light-adjustable IOLs can be adjusted with UV light after surgery to fine-tune your vision.
Sometimes, if the first IOL doesn't give the best vision, another IOL can be placed on top of it. This is called "piggyback" IOLs. It's often safer than removing the first lens.
In some countries, basic monofocal IOLs are covered by insurance. But if you choose more advanced lenses, you might have to pay extra.
During the Operation
You might start using special eyedrops (anti-inflammatory and antibiotic) a few days before surgery. On the day of surgery, your eye and the skin around it will be cleaned. A special cover will be placed over your face, with an opening for the eye being operated on. A small tool will hold your eyelid open. You will usually have local anaesthetic so you won't feel pain, but you might feel some pressure or discomfort from the bright light.
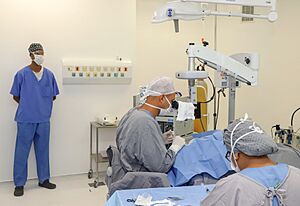
Most cataract operations are done while you are awake, using local anaesthetic. You can usually go home the same day. The anaesthetic can be given as eyedrops or as an injection around the eye. Sometimes, medicine is given to help you relax. General anaesthesia (where you are fully asleep) is usually only used for children or adults who can't stay still.
In phacoemulsification, the surgeon makes a tiny cut near the edge of your cornea. Clear, gel-like materials called OVDs are put into your eye. These help keep the eye's shape and protect it. The surgeon then makes a circular opening in the front of the lens capsule. This allows access to the cloudy lens inside.
Next, fluid is injected to separate the outer layer of the cataract from its capsule. More fluid might be used to separate the hard center of the cataract from the softer outer part. This makes it easier to break up. The cataract is then broken into small pieces using ultrasound and sucked out. Any remaining lens material is carefully removed. Finally, the folded artificial lens is put into the eye and checked to make sure it's in the right place. If it's a toric lens, it's aligned to correct astigmatism.
In MSICS, the surgeon makes a self-sealing tunnel cut in the white part of the eye (sclera). This cut is smaller than in older ECCE methods, but larger than in phaco. The lens is then removed through this tunnel. After the cataract is out, an IOL is usually put in.
ECCE involves removing almost the entire natural lens in one piece. Most of the lens capsule is left behind. This method uses a larger cut (about 10-12 mm) and usually needs stitches. It might be used for very hard cataracts or if problems come up during phaco surgery.
Sometimes, during phaco or MSICS, the surgeon might need to switch to an ECCE-like method. This happens if there are problems, like a tear in the back of the lens capsule.
After the new lens is in, the gel-like materials are removed from the eye. This prevents pressure from building up. The surgeon then seals the cut by increasing pressure inside the eye. They check to make sure the cut doesn't leak. If needed, a stitch might be added. Finally, antibiotic and steroid eyedrops are given, and sometimes an eye-shield is placed.
After the Surgery
You might need to wear an eye patch for a few hours or while sleeping for a few days. You'll use special eyedrops (steroids and antibiotics) for a few weeks. These help control swelling and prevent infection.
You should avoid getting water in your eye for about a week. Also, avoid swimming for a few weeks to prevent infection. Most people can go back to normal activities the day after phaco surgery. You should not drive for at least 24 hours after surgery.
With modern small-cut surgeries, you don't usually need to avoid lifting or bending. These activities don't typically open the self-sealing cuts. You should avoid rubbing your eyes and using eye makeup or lotions. Also, try to avoid dust, wind, or dirt. Wearing sunglasses on bright days is a good idea, as your eyes might be more sensitive to light.
Your eye will be checked to make sure the new lens is in place. Once it's stable (around six weeks), vision tests will show if you need glasses. If your IOL is for distance vision, you'll likely need reading glasses for close-up tasks.
Sometimes, people are not completely happy with their new lenses. This can happen with more complex lens designs. In rare cases, the IOL might need to be changed or repositioned. You should avoid contact sports until your eye doctor says it's okay.
What are the Benefits?
After you fully recover, how well you see depends on your eye's health and the type of new lens. More than 90% of cataract operations successfully help people see better. Serious problems are rare. The World Health Organization (WHO) suggests that after surgery, at least 80% of eyes should have good vision.
Modern calculations help doctors choose the right lens power. This means most people achieve vision very close to what was planned. This has improved over time with better equipment and techniques.
Your vision might change slightly over several years after surgery. Most of this change happens in the first year.
Are There Any Risks?
Cataract surgery is very safe and successful. But like any surgery, there are some risks. Most problems don't cause long-term vision loss.
Problems During Surgery
- Posterior capsular rupture: This is a tear in the back of the lens capsule. It's the most common problem during surgery (0.5% to 5.2% of cases). Doctors can usually fix it, but it might change how the new lens is placed.
- Suprachoroidal hemorrhage: This is a rare but serious bleeding inside the eye. It needs immediate treatment.
- Intraoperative floppy iris syndrome: This can happen if you take certain medicines. The iris (the colored part of your eye) might become floppy during surgery.
- Other problems include not removing all lens pieces or burns from the surgical tools.
Problems After Surgery
Problems after cataract surgery are not common.
- Posterior vitreous detachment (PVD): This is when the gel in the back of your eye pulls away from the retina. It doesn't directly harm vision but can increase the risk of other eye problems later.
- Posterior capsular opacification (PCO): Also called an "after-cataract." This happens when the back of the lens capsule becomes cloudy again. It can make your vision blurry. A quick, painless laser procedure (Nd:YAG laser posterior capsulotomy) can usually fix this.
- Retinal detachment: This is when the retina pulls away from the back of the eye. It's rare (about 0.5-0.6% risk after surgery), but more likely after cataract surgery. Signs include flashes of light, new floaters, or loss of side vision.
- Endophthalmitis: This is a serious eye infection. It's very rare due to antibiotic use. It usually causes decreased vision, a red eye, and pain within two weeks after surgery.
- Glaucoma: Increased eye pressure can sometimes happen. It's usually temporary. But in some cases, it can be hard to control. Children who have surgery for congenital cataracts need lifelong checks for glaucoma.
- Macular oedema: Swelling of the central part of the retina (macula). This can happen days or weeks after surgery. It can usually be treated successfully.
- IOL displacement: The new lens might move out of place.
- Unplanned refractive error: The new lens might not give the exact vision correction planned.
- Other possible issues include temporary blurry vision, double vision, or seeing a blue tint (cyanopsia).
Sometimes, a new lens might need to be exchanged or repositioned. This can happen if the lens is in the wrong place, damaged, or if you have unexpected vision problems.
Who Gets Cataract Surgery?
Access to cataract surgery varies greatly around the world. Even in developed countries, it can be harder to get in rural areas. While global eye health is improving, many people still need cataract surgery. Older people, women, and those with lower income often have more untreated cataracts.
Cataracts are a major cause of blindness worldwide, especially in poorer countries. Countries with higher incomes tend to have more eye doctors and better surgery outcomes. Lower-income countries often lack enough trained surgeons.
Europe
In 2016, about 4.5 million cataract surgeries were done in European Union countries. The number of surgeries per million people varied a lot between countries. More and more surgeries are being done as day-care procedures, meaning patients don't stay overnight.
Asia
The number of eye doctors in Asia varies widely. Some countries have many, while others have none. South Asia has a high rate of vision problems. Cataracts have been a big cause of blindness there. Even with more surgeries, some nations still have low rates.
In China, about 27% of people over 50 have cataracts. But only about 9% of them have had surgery. In India, the rate of cataract surgery has increased a lot. This is due to better techniques and more efficient clinics.
Africa
Cataracts are the main cause of blindness in Africa. They affect about half of the seven million blind people on the continent. This number is expected to grow. In 2005, about 500 cataract operations were done per million people each year. Many things make it hard for people to get surgery, like not knowing about it, not accepting it, or the cost. Women often have lower rates of surgery. Some parts of Africa have very few eye doctors.
Latin America
A study in Latin American countries showed that surgery rates increased a lot between 2005 and 2012. But many countries still don't have enough surgeries. Countries with higher incomes tend to have higher surgery rates. The main barriers are the cost of surgery and people not knowing about treatment options.
Why Cataract Surgery Matters
In 2020, about 43.3 million people were blind, and 295 million had moderate or severe vision problems. Cataracts were the leading cause of blindness.
Cataracts make it hard to see and lower your quality of life. Better vision helps with daily tasks, work, and education. Cataract surgery can also reduce the risk of falls and dementia. It's a very cost-effective treatment with big benefits for society.
The cost of surgery depends on the type of procedure and where it's done. Phacoemulsification is usually more expensive because of the equipment needed. Experts believe that standardizing procedures could reduce unnecessary costs worldwide.
Restoring vision has a huge social and economic impact. People can return to work and be more independent. Studies show it improves quality of life, finances, and mental health.
The number of people going blind from cataracts is expected to keep growing. This is because people are living longer. To help everyone who needs it, more surgeries are needed each year. Developed countries usually do enough surgeries to meet the demand. But many middle- and low-income countries still need to increase their rates.
Special Cases
Congenital Cataracts
It's very important to remove dense cataracts from young children quickly. This is because of the risk of amblyopia (lazy eye). For the best vision development, a significant cataract in a newborn should be removed before the child is six weeks old. If both eyes have cataracts, they should be removed before 10 weeks. Small cataracts that don't affect vision might just be watched.
For children older than two, the standard is to implant an IOL. For very young infants (under seven months), sometimes no IOL is put in at first. Research is ongoing into new ways to help infant lenses regenerate.
Surgery on Both Eyes
Most people with cataracts have them in both eyes. Even if one eye is fixed, having surgery on the second eye has many benefits. Sometimes, both eyes are operated on the same day. This is called immediately sequential bilateral cataract surgery. It means fewer hospital visits, lower costs, and faster recovery. It's also an option for patients who might struggle with two separate rounds of surgery. The risk of problems in both eyes at the same time is low.
Cataract Surgery in Animals
Cataract surgery is also common for pets like dogs and cats. It has a high success rate (around 90%). The procedures are similar to those for humans. Animals usually have general anesthesia.
Images for kids
See also
- Africa Cataract Project
- Eye surgery
- Himalayan Cataract Project
- IOLVIP
- Ophthalmology
- Phakic intraocular lens implantation in series with the natural lens to correct vision in cases of high refractive errors.
- Refractive lens exchange, or clear lens extraction – Effectively use of the same procedures as for cataract surgery to replace a natural lens with high refractive error when other methods are not effective.