General anaesthesia facts for kids
Quick facts for kids General anaesthesia |
|
|---|---|
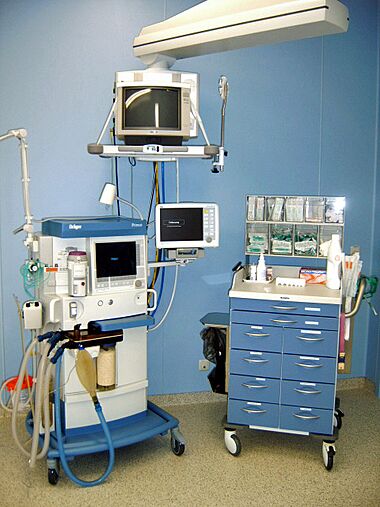
Equipment used for anaesthesia in the operating room
|
|
| Specialty | Anaesthetics |
| Uses | Helping with surgery |
| Complications | Waking up during surgery, too much medicine |
| MeSH | D000768 |
| MedlinePlus | 007410 |
General anaesthesia is a special medicine that makes a patient completely unconscious. This means they are asleep and won't feel any pain or remember anything during a medical procedure. Doctors give these medicines either through a vein (like an IV) or by having the patient breathe them in. Often, they use a mix of medicines to make sure the patient is asleep, doesn't feel pain, and their muscles are relaxed.
When a patient is under general anaesthesia, they often need help breathing. This is why it's usually done in an operating theater for surgeries. It can also be used in places like an intensive care unit to help very sick patients breathe with a machine. Sometimes, general anaesthesia is optional, but for many surgeries, it's a must. This is because even if a patient wants to be brave, their body might move or tense up during a painful part of the operation. This would make it very hard for the doctors to do their job safely.
A special doctor called an anaesthetist chooses the right mix of medicines for each patient. Their goal is to make sure the patient is unconscious, doesn't remember anything, feels no pain, and their body is still. They work with the patient and the surgeon to decide the best plan.
Contents
How Did Anaesthesia Start?
People have tried to make others unconscious for a long time. Ancient civilizations like the Sumerians, Egyptians, and Chinese all had their own ways of trying to reduce pain during medical procedures.
During the Middle Ages, smart people in different parts of the world made progress. But even with new ideas, surgery was still a last resort. It was so painful that many people chose to die rather than have an operation.
Big changes happened in the late 1800s. Scientists learned about germs and how they cause sickness. This led to using clean methods (called antiseptics) in surgery. This made operations much safer. At the same time, new medicines were discovered that could control pain. On November 14, 1804, a Japanese surgeon named Hanaoka Seishū was the first person known to successfully do surgery using general anaesthesia.
In the 1900s, general anaesthesia became even safer. Doctors started using tubes to help patients breathe during surgery. New machines helped them watch patients closely. Also, doctors and nurses began to get special training in giving anaesthesia.
Why Do We Use General Anaesthesia?
General anaesthesia is used for almost all surgeries. It helps achieve several important things:
- Unconsciousness: The patient is completely asleep and unaware.
- No Pain: The patient doesn't feel any pain during the procedure.
- No Memory: The patient won't remember what happened during surgery.
- Stillness: The patient's body stays still, which is important for the surgeon.
- Relaxed Muscles: The patient's muscles relax, making surgery easier.
Anaesthesia and Your Brain
Generally, anaesthesia does not harm your brain. However, if someone has a brain injury, like a concussion, using anaesthesia can be risky. A concussion changes how brain cells work. To fix this, the brain needs more energy. This makes the brain very sensitive during surgery. It can also affect how blood flows to the brain, which is important for getting enough oxygen. Doctors are very careful when giving anaesthesia to someone with a brain injury.
How Anaesthesia Starts
General anaesthesia usually starts in an operating room or a special room next to it. It can also be given in other places like an emergency department if someone needs urgent help.
Medicines can be given in different ways: by breathing them in, through an IV into a vein, or sometimes as a shot. Once the medicine is in the body, it travels to the brain and nervous system to make the patient unconscious.
Most of the time, anaesthesia starts either through an IV or by breathing a gas. Common IV medicines include propofol and ketamine. Breathing in anaesthesia is often used for children or if it's hard to find a vein. Sevoflurane is a common gas used because it's gentle on the throat and lungs.
Keeping You Asleep
The medicines used to start anaesthesia usually only last about 5 to 10 minutes. To keep a patient asleep for a longer surgery, doctors continue to give medicine. This can be done by having the patient breathe a mix of oxygen and a special gas, or by giving more medicine through the IV.
Often, doctors also give pain medicine, like fentanyl, and other relaxing medicines through the IV. This helps keep the patient comfortable and deeply asleep. General anaesthesia is usually very safe.
When the surgery is over, the doctors stop giving the anaesthesia medicine. The patient slowly wakes up as the medicine leaves their brain. This usually takes between 1 to 30 minutes, depending on how long the surgery was.
Waking Up After Anaesthesia
Waking up from general anaesthesia means your body and brain are returning to normal. Sometimes, patients might feel a bit confused or have trouble speaking right after waking up. Shivering is also common because the body is adjusting. This happens because the lower part of the brain (spinal cord) wakes up faster than the upper part.
Sometimes, a patient's heart rate or blood pressure might change a bit when they wake up. They might also feel a little short of breath. Doctors watch patients very closely during this time. They often ask the patient to follow simple commands, like wiggling their toes, to make sure they are waking up well.
See also
- Local anaesthesia

