Measles facts for kids
Quick facts for kids Measles |
|
|---|---|
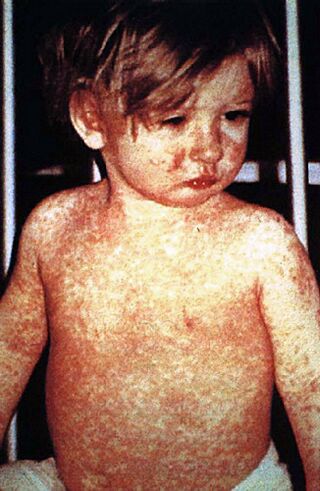
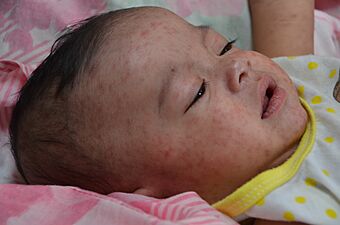
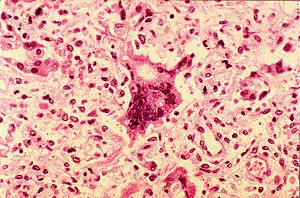
A child showing a day-four measles rash
|
|
| Classification and external resources | |
| Synonyms | Morbilli, rubeola, red measles, English measles |
| Specialty | Infectious disease |
| Patient UK | Measles |
Measles, also known as rubeola, is a very contagious illness. It is caused by a virus and can be prevented with a vaccine. Other names for measles include red measles or English measles.
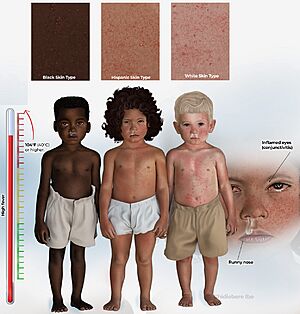
Symptoms usually appear about 10 to 12 days after someone is exposed to the virus. These symptoms typically last for 7 to 10 days. Early signs often include a fever (sometimes very high), a cough, a runny nose, and red, watery eyes. Small white spots, called Koplik's spots, might show up inside the mouth a few days after symptoms start. A red, flat rash usually begins on the face and then spreads over the whole body. This rash typically appears three to five days after the first symptoms.
Measles spreads very easily through the air. It passes from person to person when an infected person coughs or sneezes. You can also get it by touching mouth or nose fluids from an infected person. It is so contagious that about 9 out of 10 people who are not immune will get sick if they live with an infected person. People can spread the virus to others from four days before the rash appears until four days after. While often thought of as a childhood illness, measles can affect anyone at any age. Most people only get measles once in their lifetime.
There is no specific medicine to cure measles once someone is infected. However, doctors can provide supportive care to help manage the symptoms. This care might include special fluids to prevent dehydration, healthy food, and medicines to lower fever. If other infections like ear infections or pneumonia happen, antibiotics may be given. Children under 5 years old are often given Vitamin A supplements. The measles vaccine is very safe and effective at stopping the disease. It is often given with other vaccines, like the MMR vaccine.
Contents
- Where Did the Name Come From?
- Understanding Measles: Signs and Symptoms
- What Causes Measles?
- How Doctors Diagnose Measles
- Preventing Measles: Vaccination and Protection
- Treating Measles
- Measles Prognosis: What to Expect
- Measles Around the World: Epidemiology
- History of Measles
- Measles and Society
- See also
Where Did the Name Come From?
The name "measles" probably comes from Middle Dutch or Middle High German words like "masel(e)." These words meant "blemish" or "blood blister." This makes a lot of sense when you think about the main symptom of measles: a red, spotty rash that looks like tiny blemishes or blisters on the skin. So, the name simply describes what the disease looks like!
Understanding Measles: Signs and Symptoms
Symptoms usually start 7 to 23 days after someone is exposed to the measles virus. Most often, it's about 10 to 14 days. The first signs are a fever, feeling tired, and a cough. The fever can get quite high, sometimes reaching 40°C (105°F).
After two to four days, tiny white spots called Koplik's spots might appear inside the cheeks. They look like small grains of salt on a red background. These spots are a clear sign of measles, but they don't last long. The classic symptoms are a fever, cough, runny nose (like a head cold), and red eyes. Doctors sometimes call these "the three C's." A red, bumpy rash also appears. Some children might also get diarrhea after the first symptoms, which can last for up to a month.
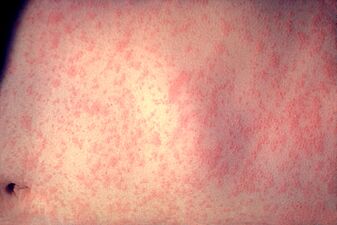
The measles rash is a red, flat, and slightly raised rash. It usually starts three to five days after the first symptoms. On average, this is about 14 days after exposure to the virus. The rash first appears behind the ears or on the face. Then it spreads to the rest of the body. The rash and red eyes happen because the body's immune system is fighting the infected skin cells. The red eyes can also make bright light uncomfortable, a condition called photophobia. Before the rash fades, it often changes color from red to a darker brown.
Most people with measles get better within days of the rash appearing. They fully recover within 7 to 10 days. A person can spread the virus to others from four days before the rash starts until four days after it appears. People with a weakened immune system might not show the rash or red eyes as clearly. This can make measles harder to diagnose in them.
Some people who have been vaccinated but don't have full protection might get a milder form of measles. This is called modified measles. It has a longer time before symptoms appear and less severe symptoms. They might have a rash but not a very high fever or bad breathing problems. They are also less likely to spread the virus.
Measles Complications: What Can Happen?
About 30% of people who get measles will have complications. Even healthy children can get very sick and need to go to the hospital. Some problems are caused by the virus itself. Others happen because measles weakens the immune system. This weakening, sometimes called "immune amnesia," makes it easier to get other bacterial infections. Studies show that after measles, the body has fewer antibodies against other germs for 2 to 3 years.
The most serious problems from measles are pneumonia (a lung infection), encephalitis (brain swelling), and blindness. About 1 to 3 out of every 1,000 children who get measles might die from breathing or brain problems. Lung problems directly caused by the virus include viral pneumonia and croup. These are more common in young children and those with weak immune systems.
Measles encephalitis can happen at any time during the illness. A very serious and often deadly brain disease, Subacute sclerosing panencephalitis, can occur years after the measles infection. This affects about 1 in 600 unvaccinated babies under 15 months who get measles. Eye problems, like ulcers on the eye, can lead to scarring or even blindness. This is worse for people who don't get enough vitamin A.
Common infections that can happen after measles include infectious diarrhea, bacterial pneumonia, and ear infections. Young children (under 5) and adults (over 20) are more likely to have complications. People with weakened immune systems, pregnant people, or those with poor nutrition also face higher risks. In countries with poor healthcare, the death rate can be as high as 28%.
Measles during pregnancy does not directly harm the baby. However, it can lead to the baby growing slowly, being born too early, or even death.
What Causes Measles?
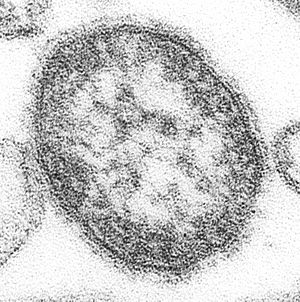
Measles is caused by the measles virus. This virus is a tiny germ that belongs to a group called Morbillivirus. It is very similar to viruses that used to infect cattle (rinderpest) and dogs (canine distemper).
The measles virus is one of the most contagious germs that affect humans. It spreads when infected people cough or sneeze. The virus can stay in the air for up to two hours in tiny droplets. It doesn't spread easily from surfaces because sunlight and heat quickly destroy it. Measles is so contagious that if one person has it, about 90% of people nearby who are not immune will also get sick. Humans are the only known natural hosts for the virus. This means it only naturally infects people, not other animals.
People are more at risk of getting measles if their immune system is weak. This can happen due to conditions like HIV/AIDS or certain medicines. Traveling to places where measles is common also increases the risk. Babies lose the protection they get from their mothers before they are old enough for routine vaccinations. This also puts them at risk.
How Doctors Diagnose Measles
Doctors usually suspect measles when someone has a fever and feels unwell about 10 days after being exposed to the virus. Then, a cough, runny nose, and red eyes appear and get worse over four days. Seeing Koplik's spots inside the mouth also helps confirm the diagnosis.
Other illnesses can look similar to measles. These include dengue fever, rubella, Fifth disease, and roseola. Because of this, doctors often recommend lab tests to be sure, especially in areas where measles is not common. Lab tests can check for measles IgM antibodies in the blood or detect the measles virus's genetic material.
Preventing Measles: Vaccination and Protection
Measles can be prevented in two main ways. One is through vaccination, which gives your body active protection. The other is by receiving anti-measles antibodies, which gives temporary passive immunity. During pregnancy, mothers can pass antibodies to their babies, giving them some protection for their first year of life. However, live vaccines are not recommended during pregnancy.
In many places, children are vaccinated against measles at 12-18 months old using the MMR vaccine. This vaccine protects against measles, mumps, and rubella. In areas where measles is common, the World Health Organization (WHO) suggests vaccination at 9 months and again at 18 months. If there's an outbreak, babies between 6-11 months might get an extra dose. The vaccine works best when given at the recommended ages. A second dose is often given between ages four and five to make sure protection is strong. Side effects from the vaccine are rare and usually mild, like a fever or soreness where the shot was given. Serious reactions are extremely rare.
The vaccine is important for all children, including those with HIV. While it might be less effective for them, early treatment for HIV can help. Measles vaccination programs often include other health services, like giving out bed nets for malaria or vitamin A supplements. This helps reduce child deaths from many causes.
Adults traveling internationally who are not sure if they are immune should get two doses of the MMR vaccine. People born before 1957 are generally thought to be immune because measles was very common then.
There have been false claims linking the measles vaccine to autism. These incorrect ideas have led to fewer people getting vaccinated. This has caused more measles cases in communities where not enough people are immune. It is important to rely on scientific evidence for health decisions.
Getting the MMR vaccine soon after being exposed to the virus can sometimes prevent measles. This is called post-exposure prophylaxis. It is usually given within 72 hours of exposure. Getting antibodies through an injection can also help for up to seven days after exposure. The MMR vaccine is 95% effective after one dose for children aged 12 months or older. After a second dose, it protects 97-99% of children.
For a community to be protected by "herd immunity", more than 95% of the population needs to be vaccinated. This is because measles spreads so easily.
Vitamin A and Measles Prevention
Not getting enough vitamin A is a big health problem in many low-income countries. It affects millions of children under five. Studies in these areas show that giving children vitamin A supplements can reduce their chances of getting measles by 50%. However, two doses of the measles vaccine provide 97-99% protection.
Vitamin A supplements are not believed to reduce the risk of death from measles. Taking too much vitamin A, especially from supplements or cod liver oil, can be harmful. It can lead to toxic levels and even liver damage.
In a measles outbreak in the Southwest United States in 2025, some families chose to give their children vitamin A supplements instead of vaccines. This was based on unscientific advice. Several children hospitalized with measles also showed signs of liver damage from too much vitamin A. Health experts strongly advise against using unproven methods for measles prevention and treatment. They emphasize the importance of vaccination.
Treating Measles
There is no specific medicine to fight the measles virus once you have the illness. Instead, treatment focuses on helping your body recover and preventing other infections. Doctors aim to keep you well-hydrated with enough fluids and to relieve pain. Medicines like ibuprofen or paracetamol (acetaminophen) can help lower fever and reduce discomfort. Sometimes, medicine to help with coughing is also given.
Some groups, like young children and those with severe malnutrition, are given vitamin A by a doctor. This helps boost the body's immune response to measles. It can also lower the risk of serious problems. While vitamin A doesn't cure measles or prevent all deaths, two doses have been shown to reduce deaths in children younger than two years old. During the 2025 U.S. outbreak, some children were hospitalized with both measles and too much vitamin A. This happened because their parents had given them high doses of vitamin A to try and prevent the illness.
More research is needed to see if zinc supplements help children with measles. Also, there isn't enough scientific evidence to say if Chinese herbal medicines are an effective treatment.
Measles Prognosis: What to Expect
Most people recover from measles, but serious complications can happen. About 1 in 4 people will need to go to the hospital, and 1–2 in 1,000 might die. Complications are more likely in children under 5, adults over 20, and pregnant people. Pneumonia is the most common cause of death from measles, accounting for 56–86% of measles-related deaths.
Other possible problems include a severe throat and airway infection (laryngotracheobronchitis) and sensorineural hearing loss. A very rare but usually deadly brain disease, panencephalitis, can occur years later. Acute measles encephalitis, which is brain swelling, is another serious risk. It usually starts a few days to a week after the measles rash appears. Symptoms include a very high fever, bad headache, convulsions, and confusion. A person with measles encephalitis might fall into a coma, and it can lead to death or brain injury.
It is rare for someone who has had measles to get it again with symptoms.
The measles virus can weaken the immune system by destroying cells that remember how to fight other germs. This can make people more vulnerable to other diseases for about two years. Historically, this weakening of the immune system may have caused more deaths than measles itself in some countries. The measles vaccine, however, uses a weakened virus and does not cause this immune system weakening.
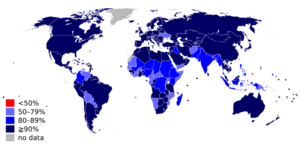
Measles Around the World: Epidemiology
Script error: No such module "owidslider". Measles is extremely contagious. For it to keep spreading in a community, new people who can get sick (like babies) must be born. If not enough new people are susceptible, the disease will eventually disappear. To achieve herd immunity, where enough people are protected to stop the spread, over 95% of a community must be vaccinated.
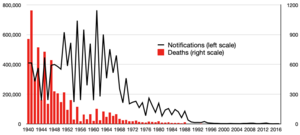
In 2011, the WHO estimated that 158,000 deaths were caused by measles. This was a big drop from 630,000 deaths in 1990. As of 2018, measles remained a leading cause of vaccine-preventable deaths globally. In developed countries, the death rate is lower, around 2 to 3 deaths per 10,000 cases. However, in communities with poor nutrition and healthcare, the death rate can be as high as 10%.
Thanks to global vaccination efforts, deaths from measles fell by 78% between 2000 and 2012. Between 2000 and 2016, global cases decreased by 84%. However, cases increased again from 2017 onwards. In 2019, there were 870,000 cases, the highest since 1996. The COVID-19 pandemic also slowed down vaccination campaigns in many countries, increasing the risk of more cases.
In 2022, about 136,000 people died from measles worldwide. Most of these were unvaccinated or undervaccinated children under 5. In February 2024, the WHO warned that over half the world was at risk of a measles outbreak. This was due to disruptions from the COVID-19 pandemic. All world regions, except the Americas, had reported outbreaks. Death rates during outbreaks tend to be higher in poorer countries.
In November 2024, the WHO and CDC reported that measles cases increased by 20% in 2023. This was mainly due to not enough vaccine coverage in the world's poorest and conflict-affected regions. Cases rose from about 8.6 million to 10.3 million. Nearly half of the major outbreaks and 64% of individual cases happened in Africa.
History of Measles

Measles originally came from animals. It evolved from a cattle virus called rinderpest. A very early form of measles might have infected humans as far back as the 4th century BC. The first clear description of measles, separate from smallpox and chickenpox, was by the Persian physician Muhammad ibn Zakariya al-Razi around 900 AD. He wrote that it was "more to be dreaded than smallpox." It is believed that the measles virus fully became a human-only virus between 1100 and 1200 AD. This matches when medieval European cities grew large enough to sustain epidemics.

Measles was an endemic disease, meaning it was always present in communities. Many people developed resistance. But in populations that had never been exposed, measles could be devastating. In 1529, a measles outbreak in Cuba killed two-thirds of the indigenous people who had survived smallpox. Two years later, measles killed half the population of Honduras. It also severely affected Mexico, Central America, and the Inca civilization.
The 1846 measles outbreak in the Faroe Islands was well-studied. Measles had not been seen there for 60 years, so almost no one was immune. Three-quarters of the residents got sick, and over 100 people died. A scientist named Peter Ludvig Panum studied this outbreak. He learned that measles spread through direct contact and that getting sick once gave you immunity. He also figured out how long it took for symptoms to appear.
Measles killed 20 percent of Hawaii's population in the 1850s. In 1875, it killed over 40,000 Fijians, about one-third of the population.
Developing the Measles Vaccine
Before vaccines, it's estimated that over 2 million deaths and 30 million cases of measles happened worldwide each year. In 1954, scientists John Enders and Thomas C. Peebles isolated the measles virus from a 13-year-old boy. They used methods similar to those for the polio vaccine to grow the virus. Their work led to a virus that could create immunity without causing the disease.
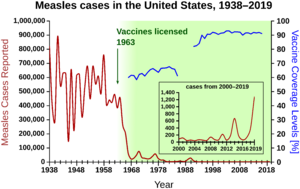
Later, at Merck, Maurice Hilleman further weakened this virus. He developed the first successful measles vaccine, which became widely available in the United States in 1963. This early vaccine sometimes caused fever and rash. To reduce these reactions, it was improved. The measles vaccine was later combined with the mumps vaccine and rubella vaccine to create the MMR vaccine. This combined vaccine was approved for use in the United States in 1971. In 2005, the MMR vaccine was combined with the varicella vaccine to create the MMRV vaccine.
Measles and Society
Measles outbreaks often happen in communities where not enough people are vaccinated. This makes the disease a way to see if a population has enough protection. Measles outbreaks have been increasing in the United States, especially in areas with lower vaccination rates. The disease is often brought into a region by travelers from other countries. It then typically spreads to those who have not received the measles vaccination.
See also
 In Spanish: Sarampión para niños
In Spanish: Sarampión para niños