Insulin facts for kids
Insulin (from the Latin word insula, meaning "island") is a special protein hormone. It is made by tiny cells called beta cells in your pancreas, which is an organ located behind your stomach. Insulin is like a key that helps your body use and store energy from the food you eat. It's the most important hormone for building up and storing things in your body.
Insulin's main job is to control how your body handles carbohydrates, fats, and proteins. When you eat, your blood sugar (glucose) levels go up. Insulin then helps your cells, especially in your liver, fat, and muscles, take in this glucose from your blood. Once inside the cells, glucose can be turned into glycogen (a stored form of sugar) or fat for later use. Insulin also stops your liver from making too much glucose and helps your body build proteins.
When insulin levels are low, your body starts to break down stored fats and other molecules for energy. This is the opposite of what insulin does.
Your beta cells are very smart! They sense how much sugar is in your blood. When blood sugar is high, they release more insulin. When blood sugar is low, they slow down insulin release. This helps keep your blood sugar levels just right. Nearby cells, called alpha cells, make another hormone called glucagon. Glucagon does the opposite of insulin: it raises blood sugar when it's too low by telling the liver to release stored glucose. Together, insulin and glucagon work like a team to keep your blood sugar balanced.
If your body doesn't make enough insulin, or if the insulin it makes doesn't work well, you can get diabetes. This is a condition where blood sugar levels stay too high.
- In type 1 diabetes, your body's immune system mistakenly attacks and destroys the beta cells. This means your body can't make insulin at all.
- In type 2 diabetes, your body might not make enough insulin, or your cells might not respond well to the insulin that is made. This is called insulin resistance.
Human insulin is a small protein made of 51 building blocks called amino acids. It has two main parts, called chains, that are connected. Insulin's structure is very similar in many different animals. For a long time, insulin from pigs was used to treat people with diabetes because it was so similar to human insulin. Today, we can make human insulin using special technology.
Insulin was the first protein hormone ever discovered! Frederick Banting and Charles Best first found it in dog pancreases in 1921. Later, Frederick Sanger figured out its exact structure in 1951. Dorothy Hodgkin then mapped its 3D shape in 1969. Insulin is also on the WHO Model List of Essential Medicines, which means it's considered one of the most important medicines for a basic health system.
Contents
Insulin's Journey Through Time
Insulin-like proteins have been around for a very long time, possibly over a billion years! They can be found in simple living things like fungi and tiny protists, not just animals.
In most animals with backbones (vertebrates), insulin is made by the beta cells in the pancreas. Some fish have a special organ called the Brockmann body that makes it. Even some venomous sea snails, like the cone snail, use a type of insulin in their venom to slow down the fish they hunt by lowering their blood sugar.
How the Body Makes Insulin
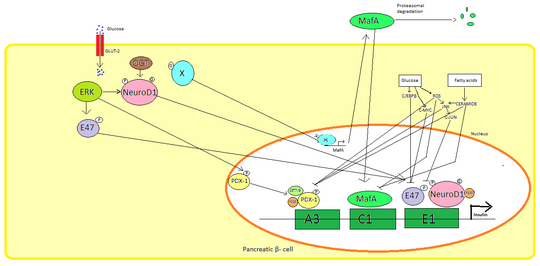
In mammals, insulin is made only in the beta cells of the pancreatic islets. The instructions for making human insulin are found in a specific gene on chromosome 11. When your blood sugar levels are high, your body tells this gene to make more insulin. This process is controlled by special proteins called transcription factors that act like switches, turning the insulin gene on or off.
Insulin's Building Blocks

Insulin isn't made all at once. It starts as a longer, inactive protein called preproinsulin. This preproinsulin then gets processed in a few steps:
- First, a small part is removed to form proinsulin.
- Then, the proinsulin folds into the correct shape, and its two main chains are connected by special bonds.
- Next, a middle section of the proinsulin, called the "C-peptide", is cut away. This leaves behind the active insulin molecule, which has its two chains connected by two bonds.
The finished insulin is then stored in tiny packages inside the beta cells, waiting for signals like high blood sugar to be released into your bloodstream.
Scientists have also found that insulin and similar proteins are made in the brain. Lower levels of these proteins have been linked to conditions like Alzheimer's disease. Other hormones, like cortisol and growth hormone, can also affect how insulin works, especially during times of stress.
What Insulin Looks Like
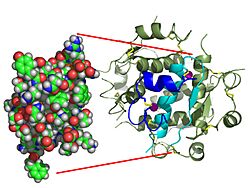
Insulin is a relatively large protein for a hormone. A single human insulin molecule is made of 51 amino acids and has two chains, called the A-chain and the B-chain, connected by special bonds.
The amino acid sequence of insulin is very similar across many different animal species. For example, insulin from cows and pigs is almost identical to human insulin. Even insulin from some fish is similar enough to work in humans! This shows how important insulin has been throughout the history of life.
Inside the body, insulin is often stored as a group of six insulin molecules, called a hexamer. But when it's time to work, it breaks apart into single molecules, called monomers. The hexamer form is very stable, which is good for storage. However, the monomer form works much faster, which is important for medicines given by injection.
How Insulin Works
Releasing Insulin
The beta cells in your pancreas release insulin in two main ways:
- A quick burst of insulin happens right after your blood sugar goes up, lasting about 10 minutes. This is like a fast response to a meal.
- Then, there's a slower, steady release of insulin that can last for a few hours. This helps keep your blood sugar stable over time.
This two-phase release helps your body manage glucose efficiently.
The process starts when glucose enters the beta cells. Inside the cells, glucose is used to make energy, which then triggers a series of steps that cause tiny sacs filled with insulin to move to the cell's edge and release their insulin into the blood.
Other things can also make insulin release, like certain amino acids (building blocks of protein) and signals from your nervous system. On the other hand, stress hormones like norepinephrine can actually slow down insulin release.
When your blood sugar goes back to normal, the beta cells slow or stop releasing insulin. If blood sugar drops too low, other hormones, especially glucagon from the alpha cells, step in to raise it by releasing stored glucose from the liver.
Insulin's Rhythmic Release
Even after a meal, insulin isn't released constantly. It comes out in small bursts, or "oscillations," every 3 to 6 minutes. Scientists think this rhythmic release helps your body's cells respond better to insulin and helps the liver take insulin out of the blood more effectively.
Blood Insulin Levels
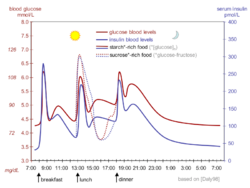
Your blood insulin level can be measured in different units. A typical level between meals is around 8–11 micro international units per milliliter (μIU/mL).
Insulin's Message to Cells
Insulin works by attaching to a special "doorbell" on the surface of cells, called the insulin receptor. When insulin binds to this receptor, it's like ringing the doorbell. This sends a signal inside the cell, telling it to open up and let glucose in.
This signal also tells the cell to store glucose as glycogen or fat, and to build proteins. It's a complex chain of events, but the main idea is that insulin acts as a messenger, telling your cells what to do with the energy from your food.
What Insulin Does for Your Body
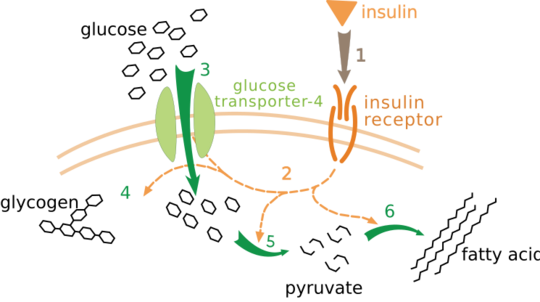
Insulin has many important effects throughout your body:
- Helps cells take in glucose: Insulin is crucial for most cells, especially muscle and fat cells, to absorb glucose from the blood. This lowers your blood sugar.
- Encourages fat storage: Insulin tells fat cells to take in glucose and turn it into fat for storage. It also stops fat from being broken down.
- Builds glycogen: When glucose levels are high, insulin helps your liver and muscles store glucose as glycogen.
- Reduces glucose production: Insulin tells your liver to stop making new glucose and stop breaking down stored glycogen into glucose.
- Builds proteins: Insulin helps cells absorb amino acids and use them to build new proteins.
- Affects blood flow: Insulin can help relax the muscles in your artery walls, which increases blood flow.
- Helps with potassium: Insulin helps cells take in potassium from the blood.
- Brain power: Insulin also enters your brain and helps with learning and memory. It can even help coordinate how your body handles food and maintains balance.
Scientists sometimes describe insulin as a "reponic" hormone, meaning it's focused on storing energy. This is different from "anabolic" hormones like growth hormone, which focus on building muscle. Insulin's main role is to make sure your body saves and stores energy from food.
How Insulin Disappears
Once insulin has done its job, it doesn't stay in your system forever. It's quickly broken down, mainly by your liver and kidneys. An insulin molecule usually lasts about an hour after it's released into your bloodstream.
Low Blood Sugar (Hypoglycemia)
Hypoglycemia is when your blood sugar levels drop too low. This can cause various symptoms like feeling clumsy, confused, shaky, sweaty, or very hungry. In severe cases, it can lead to loss of consciousness or seizures.
The most common reason for hypoglycemia is taking too much medicine for diabetes, especially insulin. It can also happen if someone with diabetes eats less than usual, exercises more, or drinks alcohol. Other causes can include kidney failure, certain tumors, or liver disease.
Conditions Related to Insulin
Several health conditions are linked to problems with insulin:
- Diabetes: This is the main condition where blood sugar levels are too high.
- Type 1 diabetes: Your body's immune system destroys the cells that make insulin, so you have very little or no insulin.
- Type 2 diabetes: Your body either doesn't make enough insulin or your cells don't respond well to it. This is often linked to diet, not being active, and being overweight, though it can happen to anyone.
- Insulinoma: This is a rare tumor in the pancreas that makes too much insulin, leading to very low blood sugar.
- Metabolic syndrome: This is a group of conditions that increase your risk of heart disease, stroke, and type 2 diabetes. It includes high blood pressure, unhealthy cholesterol levels, and a large waistline. It's often linked to insulin resistance, where your body's cells don't respond well to insulin.
- Polycystic ovary syndrome (PCOS): This is a common hormone problem in women that can cause irregular periods and other symptoms. Many women with PCOS also have insulin resistance.
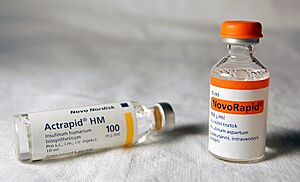
Insulin as a Medicine
Today, human insulin for medical use is made using special genetic engineering technology. This creates very pure insulin. Scientists have even found ways to grow human insulin in plants like safflower, which could make it cheaper to produce.
There are different types of insulin medicines, called insulin analogs. These are slightly changed versions of human insulin designed to work faster or last longer in the body.
- Fast-acting insulins work quickly after injection, often taken at mealtime.
- Long-acting insulins provide a steady effect for many hours, usually taken once a day to cover basic insulin needs.
- Some insulins are a mix of both fast-acting and long-acting types.
Insulin is usually given as subcutaneous injections, meaning under the skin. This can be done with single-use syringes, special insulin pens, or an insulin pump that delivers insulin continuously. Inhaled insulin is also available in some places.
Unlike many medicines, insulin cannot be taken as a pill because your digestive system would break it down before it could work.
In 2021, the World Health Organization added insulin to its list of essential medicines, highlighting its critical importance for global health. In countries like the United Kingdom, insulin and other diabetes medications are provided free of charge by the National Health Service.
The Story of Insulin's Discovery
Early Clues
The journey to discovering insulin began in 1869 when a medical student named Paul Langerhans noticed unusual clumps of cells in the pancreas under a microscope. These clumps, later named the islets of Langerhans, seemed important, but their exact job was a mystery.
In 1889, two scientists, Oskar Minkowski and Joseph von Mering, removed the pancreas from a dog. They found sugar in the dog's urine, which showed for the first time that the pancreas was connected to diabetes. In 1901, Eugene Lindsay Opie confirmed that it was specifically the islets of Langerhans in the pancreas that were responsible for diabetes.
Many researchers tried to get the special substance from these islets, but it was difficult because the pancreas also makes strong digestive juices that would destroy it.
In 1916, Nicolae Paulescu developed an extract from the pancreas that helped lower blood sugar in diabetic dogs. He published his findings in 1921. The name "insulin" was suggested by Edward Albert Sharpey-Schafer in 1916, inspired by the Latin word for "island" (insula), referring to the islets.
The Breakthrough in Toronto

In October 1920, a Canadian doctor named Frederick Banting had an idea. He thought that if he tied off the pancreatic ducts in a dog, the digestive parts of the pancreas would waste away, leaving the islets intact. Then, he could extract the special substance without it being destroyed.
In the spring of 1921, Banting went to the University of Toronto and convinced Professor John Macleod to give him a lab and an assistant. Charles Best won a coin toss to be Banting's assistant. On July 30, 1921, Banting and Best successfully isolated an extract from a dog's pancreas that lowered blood sugar.
Macleod was impressed and brought in a biochemist, James Collip, to help purify the extract even more.
On January 11, 1922, Leonard Thompson, a 14-year-old boy dying from diabetes, received the first injection of this new extract. It caused a severe allergic reaction because it wasn't pure enough. Collip worked tirelessly to improve it, and on January 23, a second dose was given. This time, it successfully lowered Thompson's blood sugar without bad side effects. This was a huge moment in medicine! Soon after, other patients like Elizabeth Hughes Gossett and James D. Havens were also successfully treated.
The drug company Eli Lilly and Company helped refine the production process, making it possible to produce large amounts of pure insulin for everyone who needed it.
Making Insulin Available to All
The discoverers of insulin faced a big decision: should they patent their discovery and make a lot of money, or should they make it available to everyone? Banting and Macleod felt it was wrong to profit from a life-saving medicine.
To prevent any single company from controlling the medicine, they decided to sell the patent for insulin to the University of Toronto for just one dollar. This meant that anyone could make insulin, but no one could have a monopoly on it. This decision was praised as a great example of medical ethics, ensuring that insulin would be affordable and accessible to people with diabetes around the world.
Nobel Prizes for Insulin
In 1923, Frederick Banting and John Macleod were awarded the Nobel Prize in Physiology or Medicine for their discovery of insulin. Banting immediately shared his prize money with Charles Best, and Macleod shared his with James Collip, recognizing their vital contributions.
Later, other scientists also won Nobel Prizes for their work related to insulin:
- Frederick Sanger won the 1958 Nobel Prize in Chemistry for figuring out the exact sequence of amino acids in insulin.
- Rosalyn Sussman Yalow won the 1977 Nobel Prize in Medicine for developing a way to measure tiny amounts of insulin in the blood.
- Dorothy Hodgkin won a Nobel Prize in Chemistry in 1964 for her work on crystallography, which she used to discover the 3D structure of insulin in 1969.
See also
 In Spanish: Insulina para niños
In Spanish: Insulina para niños